
You auscultate the chest and although there are decreased breath sounds bilaterally, there is no wheeze. 
This ‘shark fin’ pattern is classically found in two conditions: The registrar asks for help as the ventilator is alarming. 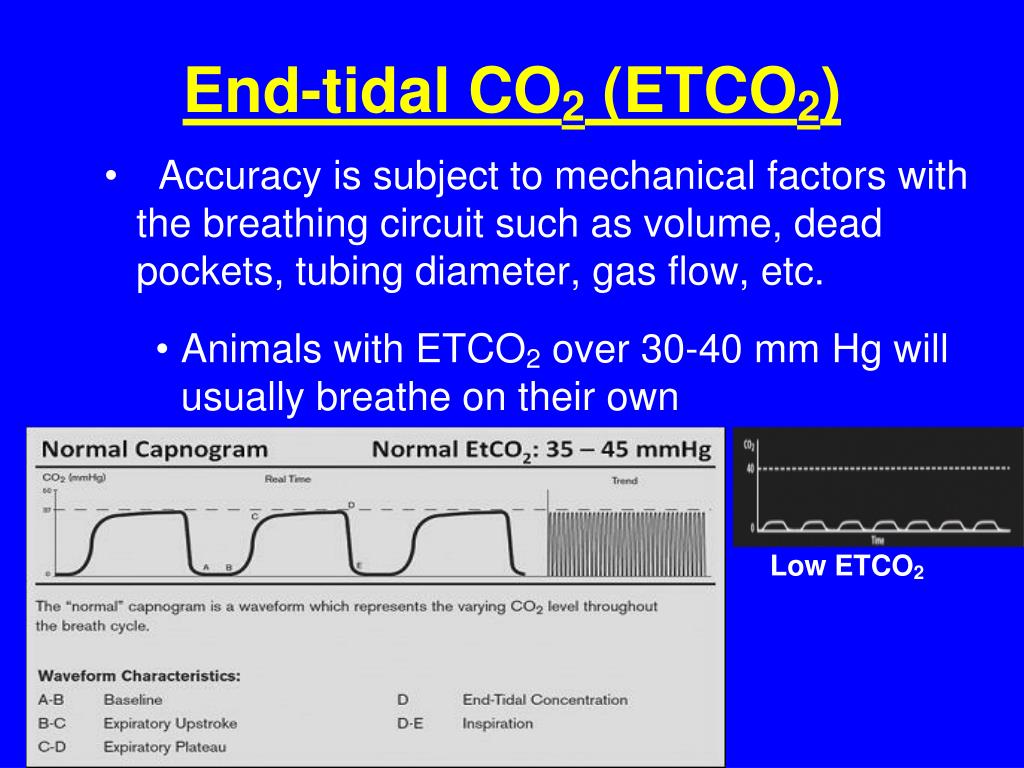
The patient is transported to the CT scanner for a brain CT.ģ0 minutes later he arrives back to the resuscitation cubicle. The Ett was pulled back 2cm and the waveform normalised to that shown below. More importantly, the patient will begin to desaturate and present an oxygenation challenge. If we wait for the chest x-ray and don’t pick this up early, it will look like this example on the left. On auscultation of the chest there is decreased air entry on the left. There is an initial reading from the right side of the lung and then the additive CO2 from the left lung. The tube is most likely, in the right main bronchus. The stepped waveform seen above is the product of two waveforms. The second intubation attempt appears to be successful. The decision is made to remove the Ett and re-intubate. There can also be chest wall rise and in about 15% of cases, breath sounds are misinterpreted as coming from the lungs when they are transmitted sounds.(1) We know that there is misting of the Ett in about 80% of cases of oesophageal intubation. Didn’t the registrar see misting of the Ett and the chest rise? Gentle bagging suction would resolve an obstruction. The same waveform can occur in an obstructed Ett, however in this case oesophageal intubation needs to be assumed. A minimum of 6 waveforms must occur, to ensure that the tube is in the right place. There is a progressive decrease in the EtCO2 waveform. This is the classic waveform produced in oesophageal intubation. There is misting of the tube and appropriate chest wall movements following intubation.Įnd tidal Co2(EtCO2) is attached and the following waveform is obtained. Using direct laryngoscopy, the experienced registrar passes the endotracheal tube(Ett). The registrar performs rapid sequence intubation, using propofol and rocuronium. The patient has been pre-oxygenated and apnoeic oxygenation has been applied. The patient’s conscious state has dropped during ambulance transport and his GCS on arrival is 7. CASES Patient 1 25 year old male brought in by ambulance following an overdose. Phase 0: This is the inspiration phase where CO2 levels drop. The height of the plateau is related to the cardiac output and the ETCO2 is measured at the end of expiration. This is due to CO2 from the alveoli now reaching the upper airway. Phase II: There is a rapid rise in CO2 as expiration continues. 
This clears the dead space where no CO2 is produced. It is the result of transport of CO2 and ventilation, its amplitude being a direct result of the level of cardiac output. The normal Range of Co2 is 35-45mmHg and this is measured at the ‘end-tidal’ point of the alveolar plateau(as described below). The waveform is a rectangular shape that has 3 phases. This moves through the body as HCO3-, until it reaches the lungs and is then expelled as CO2. As oxygen is metabolised, CO2 is produced. As it moves through the lungs into the cappilaries and end organs, it does so down a pressure gradient. The partial pressure of oxygen in air is at its highest. Gas movement occurs across a pressure differential. Ventilation: The expulsion of CO2 requires ventilation.Metabolism: Responsible for the production of CO2.Below are 3 cases, where we look at some of the potential waveforms we might encounter in the intubated patient in the emergency department. Understanding capnography and being able to decipher the waveforms, can give us critical information on a patient’s condition, early.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
